Your family doctor may suspect BPPV from the symptoms you are describing, since it is very commonly triggered by things like rolling over in bed, getting in and out of bed, tipping the head to look upward, bending over, and quick head movements. There may also be a correlation with one’s preferred sleep side 4. However associations have been made with trauma, migraine, inner ear infection or disease, diabetes, osteoporosis, intubation (presumably due to prolonged time lying in bed) and reduced blood flow. The vast majority of cases occur for no apparent reason, with many people describing that they simply went to get out of bed one morning and the room started to spin. It is thought to be extremely rare in children but can affect adults of any age, especially seniors. Who Is Affected?īPPV is fairly common, with an estimated incidence of 107 per 100,000 per year 2 and a lifetime prevalence of 2.4 percent 3. By alerting your healthcare provider to symptoms you are experiencing in addition to vertigo they can re-evaluate your condition and consider whether you may have another type of disorder, either instead of or in addition to BPPV. Other disorders may be initially misdiagnosed as BPPV. If you have any of these additional symptoms, tell your healthcare provider immediately. It will NOT affect your hearing or produce fainting, headache or neurological symptoms such as numbness, “pins and needles,” trouble speaking or trouble coordinating your movements. It is important to know that BPPV will NOT give you constant dizziness that is unaffected by movement or a change in position. Between vertigo spells some people feel symptom-free, while others feel a mild sense of imbalance or disequilibrium.Ĭheck out the American Academy of Otolaryngology-Head & Neck Surgery’s BPPV Clinical Practice Guidelines. This false information does not match with what the other ear is sensing, with what the eyes are seeing, or with what the muscles and joints are doing, and this mismatched information is perceived by the brain as a spinning sensation, or vertigo, which normally lasts less than one minute.

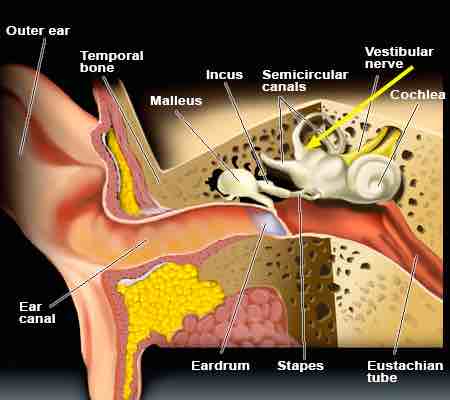
When the fluid moves, nerve endings in the canal are excited and send a message to the brain that the head is moving, even though it isn’t. However, the crystals do move with gravity, thereby moving the fluid when it normally would be still. Hain.įluid in the semi-circular canals does not normally react to gravity. Image adapted by VeDA with permission from T. The detached otoconia shift when the head moves, stimulating the cupula to send false signals to the brain that create a sensation of vertigo. Otoconia migrate from the utricle, most commonly settling in the posterior semicircular canal (shown), or more rarely in the anterior or horizontal semicircular canals. Tinnitus disappeared or decreased in all patients except two, either spontaneously, before performing the therapeutic manoeuvers, or shortly after.Ī possible vestibular origin of tinnitus determined by the detachment of macular debris into the ductus reuniens and cochlear duct is discussed.Figure 1: Inner ear anatomy.

It was mostly unilateral, localized on the same ear as the BPPV, slight in intensity and intermittent. Those suffering from tinnitus were also assessed using visual analogue scales and tinnitus handicap inventory.ġ9.3% of the patients reported the appearance of tinnitus concurrently with the onset of the positional vertigo.

The aim of this study was to describe the prevalence and the clinical patterns of tinnitus episodes which occurred in association with BPPV and to suggest possible interpretative hypotheses.ġ71 normal hearing patients affected by BPPV (50 males and 122 females age range: 25-77 years mean age 60.3 years ± 14.9) underwent pure tone audiometry, immittance test and a clinical vestibular evaluation before and after repositioning manoeuvers. In our clinical experience, some of the patients affected by benign paroxysmal positional vertigo (BPPV) reported the onset of tinnitus shortly before or in association with the positional vertigo.
